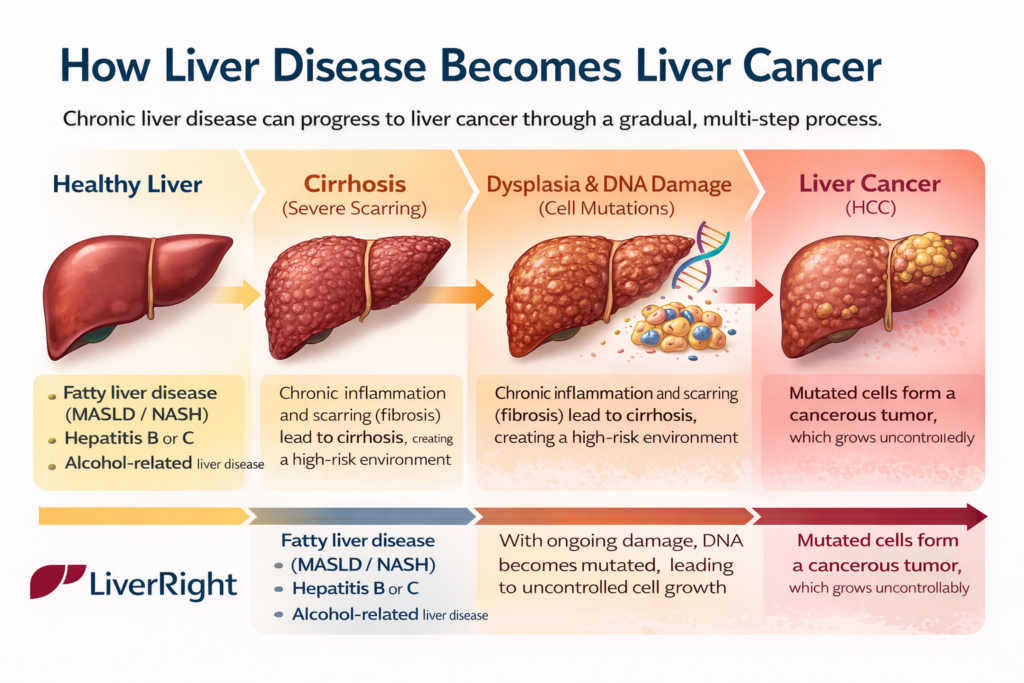
Liver disease can turn into liver cancer through a gradual, multi-step process driven by chronic damage, inflammation, and cell mutation. Here’s the clearest way to understand it:
1. Chronic liver injury starts the process
Common causes:
- Fatty liver disease (MASLD / NASH)
- Hepatitis B or C
- Alcohol-related liver disease
These conditions continuously damage liver cells over years.
2. Inflammation and scarring (fibrosis → cirrhosis)
As the liver tries to repair itself:
- It forms scar tissue (fibrosis)
- Over time, this can progress to cirrhosis (severe scarring)
Cirrhosis creates a high-risk environment for cancer because:
- Normal liver structure is disrupted
- Cells are constantly dying and regenerating
3. DNA damage and mutations
With ongoing inflammation:
- Liver cells divide more հաճախ to replace damaged cells
- This increases the chance of genetic mistakes (mutations)
Some mutations:
- Allow cells to grow uncontrollably
- Prevent normal cell death
- Disrupt tumor-suppressing mechanisms
4. Development of liver cancer (Hepatocellular Carcinoma – HCC)
Eventually:
- A group of mutated cells begins to grow independently and uncontrollably
- This forms a tumor → liver cancer
Key insight
👉 Most liver cancers don’t appear suddenly — they develop after years (or decades) of silent liver disease.
Important nuance
- Cirrhosis is the biggest risk factor, but cancer can sometimes develop before cirrhosis (especially in hepatitis B or advanced fatty liver disease).
- Early liver disease is often silent, which is why many people are diagnosed late.
Why this matters (especially in real-world care)
The progression looks like:
Healthy liver → Fatty liver → Inflammation → Fibrosis → Cirrhosis → Cancer
Catching people earlier in that chain dramatically lowers cancer risk.
